You would think that Leprosy was a disease of the past, predominantly during the Medieval Period, right? Well think again.
When I travelled in Nepal I saw first hand people with classic telltale signs of leprosy. Blinded by the disease, they were begging for money on the streets, stretching their fingerless hands out for coins or food, their toeless feet, half hidden under their robes. Prior to that I had been in Bergen and visited the leprosy museum, surprised to find that there were colonies of people with leprosy in Bergen well into the 20th century. With my background as an anthropologist I was well aware of people in the archeological record having lived with leprosy. I was not aware of people still living with the disease or how wide spread it was. This triggered me to look into leprosy and write this piece for my blog.
In 2018 alone there were more than 200.000 new cases of people being diagnosed worldwide, with countries such as Brazil, India and Indonesia having the largest populations of people with leprosy. This number means that about 0.2 per 10.000 worldwide is diagnosed. The World Health Organization (WHO) has said that leprosy is no longer a public health issue, with less than 1 case per 10.000 people being diagnosed. Worldwide it is estimated that currently more than 7 million people are suffering from leprosy.
Leprosy is also present in developed countries, such as the UK and US with more than 1500 individuals living today with leprosy alone in the UK, predominantly being immigrants contracting the disease in their home countries.
In North America, due to its larger population mass there is an even larger infected population. However, in the USA leprosy is generally contracted not from immigrants bringing the illness with them from their home countries, but from a totally different source; the bacterium causing leprosy can be found on the armadillos in southern states such as Texas and Louisiana. The bacteria thrive at the specific temperature of 32-35 degrees – which is the body temperature of the nine-banded armadillo and therefore make it an ideal carrier of the disease. This is also why the skin damage in humans is seen in the cooler areas of the nose and extremities. Interestingly, the leprosy strain is only carried by the nine-banded armadillo and not the three- or seven-banded armadillo. About 30-50 people a year are thought to have contracted the disease locally in USA from the armadillo. Just recently, leprosy was also found in nine-banded armadillos in Brazil where leprosy is spread from armadillos to humans due to hunting them as a food delicacy.
How contagious is leprosy?
Contrary to beliefs, leprosy is not very contagious, only being considered “mildly contagious”. To contract the disease you would in generally need long-term contact with a person with leprosy, ranging from months to years. Infection transference may also occur through respiratory droplets, for example, coughing.
It is estimated that more than 95% of people who are infected with Mycobacterium leprae do not develop leprosy because their immune system fights off the infection. People who do develop leprosy may have a genetic background that makes them susceptible to the infection once they are exposed.
Leprosy is caused by the bacteria, Mycobacterium leprae, that favors nerves and skin in cooler areas. Symptoms do not typically present until 5-20 years after infection, with the first signs being patches of lighted colored skin (see Fig. 1) with a reduced sensation to touch and ‘pins and needles’.
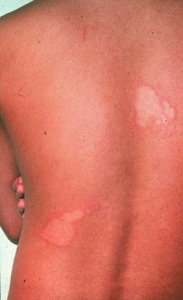
Fig. 1: Early signs of leprosy. Image: Fisher 2014 (full reference below).
Later, you would start to feel a weakness in your hands and feet, numbness, joint pains followed by skin sores. In the later stages, when nerve damage has set in, hair loss will show together with a loss of fingers (see Fig. 2) and toes and collapse of the nasal bridge with anterior dental loss. Eye damage from dryness may lead to blindness.

Fig 2: later affects of leprosy with loss of fingers due to nerve damage. Image: The Leprosy Mission, NI (full reference below).
In modern days, once diagnosed in humans, leprosy is easily managed with multidrug therapy. From the first day of treatment, the patient can no longer contaminate others with leprosy. For people with advantaged stage infection that have caused facial disfiguration, reconstructive surgery (Fig. 3) can be performed to diminish the visual stigma surrounding leprosy.
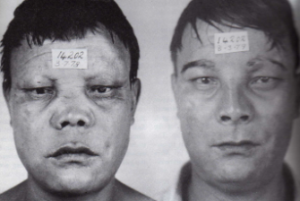
Fig. 3: Before and after reconstructive surgery for leprosy. Image: Brand, 1983 (full reference below).
In the advanced form, which you would see without treatment, leprosy can be seen on the skeleton, particularly to the face, hands and feet (see Fig. 4). It is from the skeletal record that we know that leprosy has existed as far back as 4000 years, with the earliest case found in a male skeleton from India, dating to about 2000 BC.
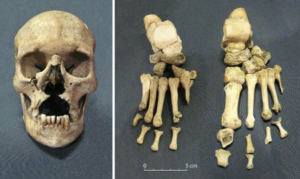
Fig. 4: Skull and feet showing typical leprosy changes. The skull (left) show destruction of the lower nasal area and the the upper jaw. The feet (right) show absorption of the distal part of most toes and thinning of other foot bones. Images: Professor Eileen Murphy, Queen’s University Belfast (full reference below).
Historical records show that leprosy affected rich as well as poor, with the most notable of cases such as King Baldwin IV who was King of Jerusalem during the periods of the crusades. He died at the age of 24 in 1185AD, severely disfigured and blinded from leprosy. As leprosy takes many years to develop to this stage he is likely to have contracted the disease during childhood.
The Scottish King, Robert the Bruce, has also been considered to have had leprosy. King Robert the Bruce successfully fought for an independent Scotland, notably at the Battle of Bannockburn in 1314 where after he was King until his death in 1329. When he died he had been ill for many years. There have been persistent rumors that he suffered from leprosy, which have still not been settled despite several examinations of a plaster cast made from his skull when his remains were exhumed in 1818.
Often people suffering from leprosy were put in isolated communities to seperate them from the healthy people. Examples of these leprosy communities are known from excavations of medieval leprosariums (hospitals or communities that provided care for people suffering from leprosy). One of the latest known leprosariums in northern Europe was in Bergen, Norway. In fact, Bergen had three leprosariums between 1850 and 1900 with the largest concentration of leprosy patients in Europe. In 1946 the last two patients died and the hospital closed.
Interestingly, leprosy has also been found in the red squirrel populations (Fig. 5) in the UK. However, again, it is only in one variant of squirrel, namely the red and not the gray squirrel. Although in the UK, the red squirrel has not been found to infect humans and the risk thereof is considered negligible. The origin of leprosy in the UK squirrel population is currently believed to derive from Viking trade with fur of the red squirrel.

Fig. 5: Red squirrel with leprosy changes showing on the nose area and ears. Image: Karen van der Zijden (full reference below).
What does the future of leprosy look like then? Even though as mentioned in the beginning, that WHO no longer considers leprosy as public health issue, there is still a strong concern to manage this illness better. In 2016, 2017 and 2018 major reports were issues by WHO to help affected countries develop a strategy for management through early diagnosis, treatment and thereby minimise new cases of leprosy.
References for images:
Fig. 1: Fisher, M. 2017. Leprosy – an overview of clinical features, diagnosis, and treatment. Journal of German Society of Dermatology, 15(8), pp. 801-827.
Fig. 2: The Leprosy Mission, Northern Ireland. Website: https://www.tlm-ni.org Accessed January 2020.
Fig. 3: Paul W. Brand. Rehabilitation in Leprosy. Leprosy 1983. Accessed here: https://web.stanford.edu/class/humbio103/ParaSites2006/Leprosy/treatment.htm
Fig. 3: Taylor GM, Murphy EM, Mendum TA, Pike AWG, Linscott B, Wu H, et al. (2018) Leprosy at the edge of Europe—Biomolecular, isotopic and osteoarchaeological findings from medieval Ireland. PLoS ONE 13(12): e0209495. https://doi.org/10.1371/journal.pone.0209495
Fig. 5: Leprosy revealed in red squirrels across British Isles. The Gaurdian. Accessed here: https://www.theguardian.com/environment/2016/nov/10/leprosy-revealed-in-red-squirrels-across-british-isles
Hvor er du god?jeg vidste ikke at stadig så mange var syge. For 2 år siden så ruiner af ruiner på Bornholm, hvor de isolerede de syge i gamle dage. Men hvis bakterierne trives i varmen, hvorfor var der så mange syge i Norge?
Dear Katarina,
Thank you for reading the blog post and taking your time to ask the question: “If the bacteria thrive in warmth, why was there so many ill in Norway?” (I hope I have translated your question correctly!)
The bacteria itself thrive in temperatures of around 32-35 degrees, which is why you most often see it manifested in the cooler areas of the body such as the extremities (finger and toes) and the face. If you mean why it is prevalent in the warmer geographical areas such as Brazil and India today, then this is to do with access to treatment – often people do not know there is treatment, or how to access it (due to illiteracy), or access to treatment is prevented due to travel distance (and cost thereof). Why Norway had leprosy increasing during the 18th century, has by historic sources been explained by the great poverty that Norway experienced then. After the Napoleonic wars, the breakdown of the Danish- Norwegian state in 1814 and the subsequent transfer of rule to Sweden, caused significant increased poverty in Norway, and has been suggested as a contributing factor for the increase in leprosy in the 18th century. When the living conditions of the country improved, leprosy started to decline until it became eradicated.
Hope this answered your question!
Best wishes from
Charlie